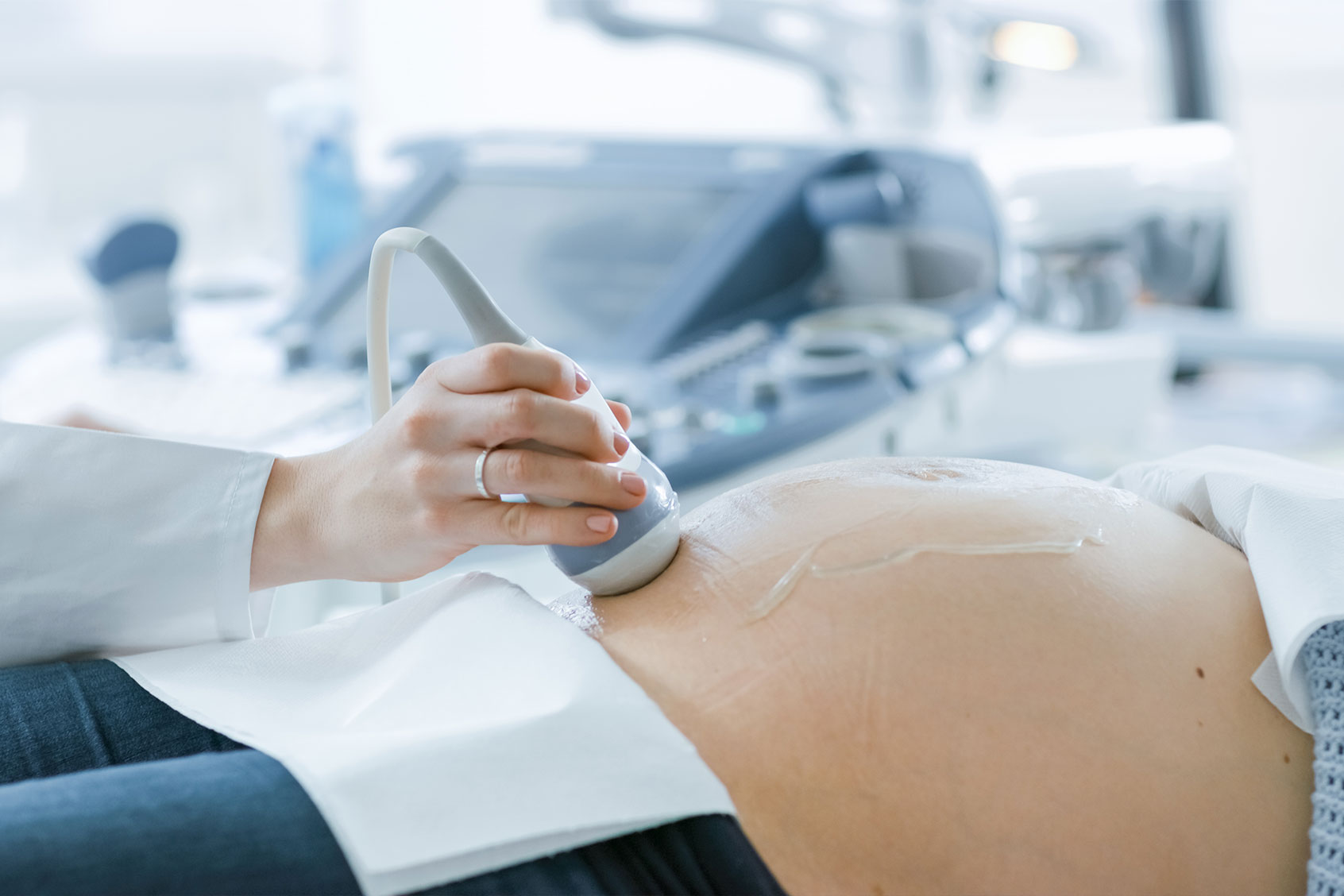
How a “selective reduction” abortion saved my child’s life
I’m lying on an exam table, on that crinkly, uncomfortable paper known only to doctor’s offices. A lumpy vinyl pillow supports my head. Monitors hang from the ceiling above me. Various obstetric and gynecological tools sit and stand around the room. The room is cold and austere.
Some enterprising interior designer tried to soften the harshness of the room with strategically-placed artwork. I can’t remember what the art was, except that it was there, and I remember thinking it was a nice attempt; but if they were trying to soften this reality, I would have much preferred a nice Valium instead of mass-produced department store art.
Not that Valium was an option.
It is 8 a.m. on August 2, 2019, at a building in Mount Sinai Hospital in New York City. I am 14 weeks pregnant with three babies — a set of identical twin girls and a fraternal boy. I am about to undergo a procedure called “selective reduction,” which will terminate the identical twins I am carrying and leave their brother safely behind.
The fact that I am pregnant at all, let alone with triplets, feels impossible after five years of inexplicable infertility. After countless medications, procedures, and various assisted reproduction technologies, the doctors concluded that using my eggs was unlikely to result in having a child. We chose to use donor embryos because they seemed like the most likely path to success for us. We wanted our baby. We were more than ready.
At our seven-week ultrasound, the doctor said, “Hmm, I think I see… Never mind. It’s a shadow. I thought I saw another baby.”
I went through a medication cycle to prepare my body for embryo transfer. We had two embryos, and, given our history, our doctors advised transferring both. The chances of one embryo “sticking” were 60%. The chances of both: 40%. The possibility that one of them would stick and split, becoming twins? Less than 2%. A few days later, I saw two strong, beautiful pink lines — lines I’d dreamed of all my adult life. A blood test confirmed that I was pregnant. Very pregnant, apparently. My beta numbers were off the charts. “I’ll be interested to see how many you’ve got in there,” the nurse mused. We assumed twins. At six weeks, my first ultrasound indeed showed two sacs. We were thrilled.
At our seven-week ultrasound, the doctor said, “Hmm, I think I see… Never mind. It’s a shadow. I thought I saw another baby.”
I started bleeding a few days later. Fearing a miscarriage, we rushed back to the doctor. Aghast, she looked up from the screen: “You’ve got three in there.” She immediately referred us to a maternal-fetal medicine doctor. This was not good news.
After years of worrying we would never have children, now, in some cruel twist, we were being asked to choose to terminate two of them.
Time became sticky, a physical thing I could reach out and touch. Its edges shrunk to smother me and then sped away. I stood in a timeless void filled with nothing but the sound of our four heartbeats and the improbability of the situation: Triplets. It took a week to get in to see the specialist. My belly grew quickly: I started my pregnancy athletic and slim, and the three babies needed room to grow. By eight weeks, I had a small bump. Most people don’t even need to buy maternity clothes for months, but I did by eight weeks. I could feel little flutters.
We consulted with multiple specialists. All said the same thing: You need to reduce the twins. They are sharing a sac. One of the twins is already showing signs of slowed growth.
My husband and I had never even heard of the term “selective reduction.” After years of worrying we would never have children, now, in some cruel twist, we were being asked to choose to terminate two of them.
What is selective reduction?
Selective reduction is a procedure to stop the development of one or more fetuses in utero (ACOG). Dr. Mark Evans pioneered the procedure in the 1980s, collaborating closely with Drs. Richard Berkowitz and Ronald Wapner. Speaking by phone, he told me about the call he received from a colleague that led to the first selective reduction procedure: A woman in Western Michigan had become pregnant with quadruplets. She was 4’10”. Her doctor said there was no chance for her to carry them to term. Could Dr. Evans, a known innovator in fetal medicine and therapy, perform half an abortion? This led to Dr. Evans performing the first selective reduction, reducing the quadruplets to twins. They’re now in their thirties.
Shortly after, he received another call: A woman in Alaska was pregnant with octuplets. Dr. Evans reduced the pregnancy from eight to two. These children are also alive and in their thirties. Since then, Dr. Evans has performed this procedure for thousands of women from all over the world, devoting his career to helping women. “My goal,” he says, “is a healthy mother and a healthy family. That’s it.”
Experts recommend that fetal reduction take place between 12 and 14 weeks — before 12 weeks, there is a higher risk of miscarriage.
Why reduce?
Before multifetal pregnancy is even considered, pregnancy with a single baby can be risky business in the United States. Compared with other wealthy countries, the United States has the highest maternal mortality ratio — even when that data is limited to only white women, typically the most privileged group.
States including Alabama, Arkansas, Kentucky, and Oklahoma reported maternal mortality ratios greater than 30 per 100,000 live births. Those are terrifying data to consider, particularly given that these are real birth mothers’ lives.
Women can die during pregnancy or childbirth for all kinds of different reasons; multifetal pregnancies increase these risks. Unfortunately, these risks remain higher than average for the mother even after reduction — but still lower than if it isn’t.
Mom isn’t the only one at risk. Multifetal pregnancies increase the risk to the babies, whether the fetuses are healthy or not, and these risks only increase with the presence of each additional fetus — even for twins. And the risk of spontaneous loss for the entire pregnancy is 25% for quadruplets, 15% for triplets, and 8% for twins.
Risks to the fetuses in high-order pregnancies include “intrauterine growth retardation, respiratory distress syndrome, miscarriage, and preterm delivery.” Compared to singleton pregnancies, multi pregnancies are approximately five times more likely to result in stillbirth and seven times more likely to result in neonatal death. Along with prematurity, which has complications, multifetal pregnancies have increased risks of cerebral palsy, children having learning disabilities, slower language development, chronic lung disease, developmental delays, and death.
The risk of selective reduction for the mother is low; statistics from the Pregnancy Mortality Surveillance System of the Centers for Disease Control and Prevention show that 0.0009% of women in the United States died from legal abortions, including selective reduction procedures.
Risks for the remaining fetus(es) are often lower with selective reduction than if the pregnancy continues with higher multiples. Certain fetal pathologies, like cord entanglement or twin-to-twin transfusion syndrome, risk the development and survival of the other babies.
Difficult choices — but our choices
People ask, how do you choose? It’s not always clear — or easy.
“Sometimes you have to do unpleasant things to get the right result,” Dr. Evans says. I agree. Dr. Evans says, in his experience, about 50% of the time, women choose to reduce. Either way, it is always their choice.
In my case, our doctors said I was guaranteed preterm labor — or, as one put it, “You’ll be lucky to make it to 28 weeks.” The babies would be at least 12 weeks — three months — early.
Elizabeth chose selective reduction. “Having already buried a child due to a genetic condition, I couldn’t go through that again, and it wouldn’t have been fair to my other living children,” she said. “I made the gut-wrenching decision to be here for all of them versus losing one, or two, or three of them.”
In my case, our doctors said I was guaranteed preterm labor — or, as one put it, “You’ll be lucky to make it to 28 weeks.” The babies would be at least 12 weeks — three months — early.
We also had a 40% chance that all or some of the babies would be born with profound congenital disabilities. There were significant chances the twins would have issues as the pregnancy progressed, including the one twin’s slowed and possibly completely stopping growth, or twin-to-twin transfusion, where one twin would leech all the nutrients and leave the other baby with nothing. And there were the ever-present risks a higher-order triplet pregnancy presented.
It felt profoundly unfair, a deal with a devil: Yes, you can carry and have a child, but in return, you will suffer an unknowable pain.
The decision was complicated. It involved my health, my feelings about my body, carrying children, women’s autonomy, our family’s future, my husband’s feelings, his worry for my health, and the health of our babies. We worried about what we would tell the surviving baby when they got older. We feared we would have regrets. We worried we would lose them, any and all of them. We worried we would lose each other. We worried we would lose ourselves. The lives we had built, the expectations we had for the future. Our careers, our home, the next sixty years — for us, for them.
It felt profoundly unfair, a deal with a devil: Yes, you can carry and have a child, but in return, you will suffer an unknowable pain.
We made a choice. We had to.
But it was not made lightly.
Dr. Evans likens it to the lifeboat phenomenon: Sometimes, sacrifices are needed and legitimate when the interest of the many outweighs the few. Sometimes the choice is bleak: You can save some, but you cannot save all. But, you do get a choice.
You can choose to save some or to sink the whole boat — that is a choice, too.
Elisabeth also chose to reduce — it was the right choice for her family. “I would have lost my entire pregnancy, and instead, I have two healthy, thriving 9-year-olds. I knew in my gut that I needed to do this to save them. I was right. Women know our own bodies — if you expect us to be mothers, you must trust our judgment and our decisions about our bodies and our lives,” Elisabeth says.
Medical procedure — not a crime
Dr. Evans asked: “If you told someone they had cancer, and one treatment had a six percent mortality rate, and one had a two percent mortality rate, would you judge them for taking the one with the lower mortality rate? Of course not.”
Yet, to be a woman in the United States is to be judged. When it comes to conception, pregnancy, and motherhood, that includes the unchecked opinions of everyone you encounter on how you should mother. My husband certainly never had to deal with strangers sending him anonymous Bible verses and death threats about this decision, or questioning his ability to be a father.
That was all reserved for me.
Sadly, many of the women I’ve met through this experience choose not to share their selective reduction with anyone outside of their immediate or close family. Anya said, “The fact that it isn’t widely supported or understood in my state and by my religious extended family meant alienation and a sense of shame that wasn’t necessary and didn’t help navigating what was already a very difficult decision. I know for a fact that if I hadn’t reduced, I would have lost my pregnancy. It was his (Dr. Evans) reassurance that enabled us to have a family versus losing it all.”
When I learned I needed a selective reduction, I turned to the internet. I expected social media groups, articles, and interviews. There were a couple of articles and lots of academic papers. I found zero support groups, the reason for which became apparent as I started writing about and sharing my story, first through the People interview. Some people really, really hate anything that looks like an abortion, even if it’s the thing that saves your life or your other baby’s life. Shawna was called a murderer when someone found out she received a reduction. Even with the reduction, her boys were born three months early. “We all almost died,” she said. “I lost a ton of blood.”
Eventually, a woman reached out to me from a social media group that operates like the Aunties network from the Handmaid’s Tale — you have to be invited in, you have to be vetted, you have to be approved. Why? Because this is a dangerous world for women who make choices about motherhood.
I found solidarity with these women. And, they found solidarity with me. A week hasn’t passed since I started sharing my story that a woman hasn’t reached out to me to say that she, too, has been blindsided by the possibility of selective reduction, and she, too, doesn’t know where to turn. We connect, and I help her find the nearest resources, and if she wants, I invite her to the group. It’s a good feeling to find other people who have been faced with one of the worst decisions, one of the most horrible life events you can imagine.
I call it the Terrible Sisterhood.
Saying the A-word: does it matter what you call it?
So, is selective reduction abortion? Selective reduction and abortion both involve terminating fetal life, yet they’re different medical procedures performed by different physicians and possibly for different reasons. However, in the minds of many in the anti-abortion camp, the distinctions don’t matter.
In that sense, they’re right: It doesn’t matter — because it shouldn’t matter. Lawmakers should not get to make decisions about what a woman carries in her womb or when. Choosing to have a child or multiple children is the most significant life change one can make, affecting every relationship, decision, expenditure — everything that family touches for the rest of their lives.
Whether or not selective reduction is abortion, however, is now an important matter of distinction. The Supreme Court has overturned Roe v. Wade in the Dobbs v. Jackson Women’s Health Organization decision — and we don’t know what that will mean yet for selective reduction, particularly for the women and families who live in states where access will be further restricted.
When I started trying to get pregnant, I didn’t think I’d have to utilize assisted reproductive technology like IVF, let alone donor embryos. And when I transferred two donor embryos, the last thing on my mind was that I would have to reduce two extremely wanted fetuses.
But it happened. It happened to me, it happened to hundreds of women I now know, and it will continue to happen despite the court’s decision — it will just become even more difficult for people to access care. Anya, for example, had to travel out of state to see Dr. Evans.
“The fact that it wasn’t available in my state meant that I had to incur travel expenses that I couldn’t afford and the stress of finances and travel in addition to the stress of the decision and procedure itself,” she said.
Choice is justice
If you’re concerned about protecting life, the way to do that is by protecting access to safe and quality healthcare and supporting the women and families seeking it. This is healthcare. Women require access and support. No one should lack access to necessary resources, or be shamed, because biology happens. No government should mandate how a person chooses to handle their own biology.
The science is clear: Pregnancy itself is risky, and higher-order multiple pregnancies are even more so. My triplet pregnancy required a choice.
Even after choosing the selective reduction, I still had complications with my remaining baby: I had a shortened cervix starting around 20 weeks. I was diagnosed with Deep Vein Thrombosis at the beginning of my third trimester, leading to hospitalization. I had a filter installed into my vena cava so that the clot wouldn’t move. I was on blood thinners for the remainder of my pregnancy and six months beyond.
My son was born at 37 weeks and one day. Despite the reduction, he was still early. There were still complications.
And I did deliver the twins. After 23 more weeks in the womb, physically, they were little more than tissue. But, as I held my son on my chest and our tears mingled for the first time, some of them were for his sisters, too. I was relieved. I was overjoyed. And I grieved, too. I am a mother of three, with one living son. Things could not have been different. I do not regret my choice. And yet, I catch my breath when I hear someone speak their names.
I wish I had gone through the entire experience with the support of a community, and a society, that valued and understood the science of reproduction. My wish, moving forward, and the reason I keep talking about it and keep bringing attention to it, is that we live in a society that values, understands, and respects the health and autonomy of our women.
Selective reduction was not an easy choice. But it was my choice.
Women deserve to be supported in that choice. We deserve a society that recognizes — and embraces — reproductive justice.
Read more
on reproductive justice