Celebrities are talking openly about menopause. Why won’t the healthcare industry?
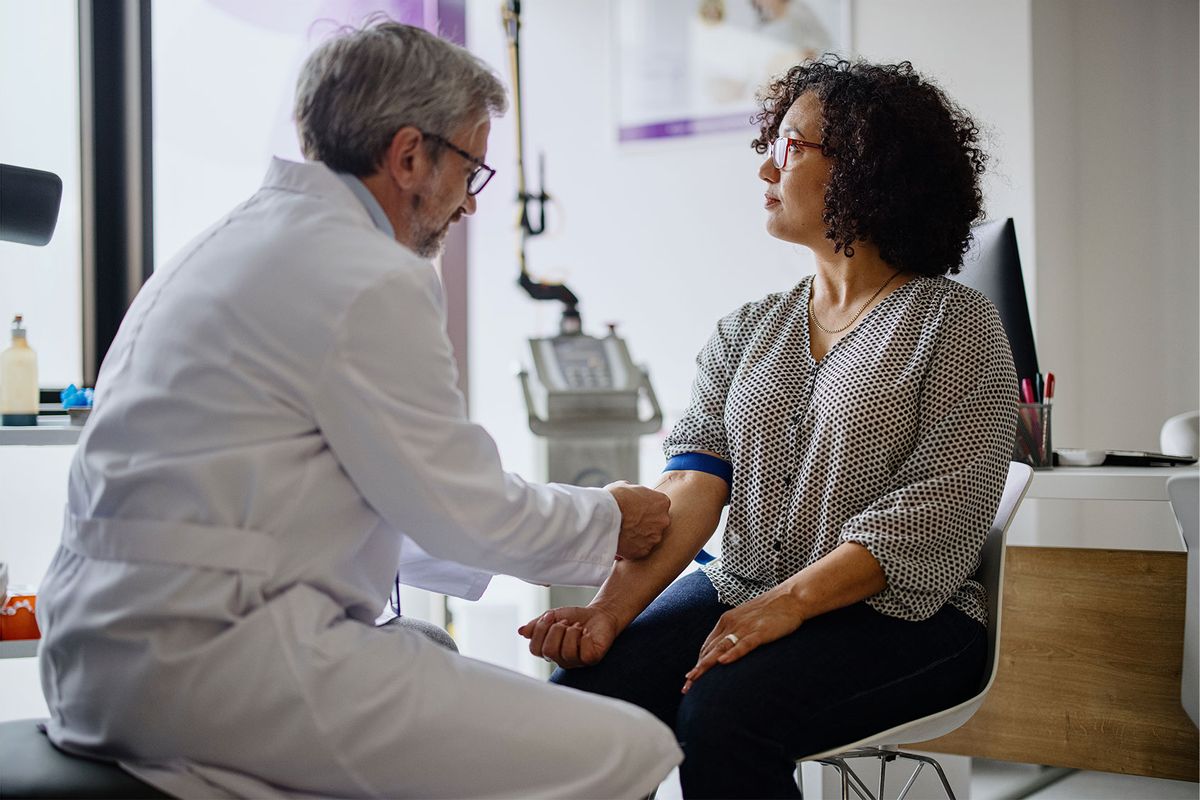
Menopause wasn’t always a topic that was talked about loudly, on talk shows and brunch joints. But that appears to be changing (finally), as a number of public figures are opening up about what used to be a private, deeply personal topic. Recently, Oprah sat down with Drew Barrymore, Maria Shriver, and menopause experts to discuss her perimenopausal heart palpitations, brought on by decreased estrogen and progesterone. These women join a growing cadre of public figures, including Gayle King, Naomi Watts, Stacy London, and Michelle Obama, who are helping to shift the narrative around women’s bodies, health, and aging.
In some ways, the sheer exuberance of these conversations-between-friends–style segments hints at a marked change in perspective. The frank discourse around women’s health issues — particularly that of older women — is long overdue.
Why aren’t doctors and oncologists better preparing us, their patients, for what to expect in menopause?
Yet I can’t help but notice that the current dialogue is falling short. Too often, these orchestrated sit-downs become a jolly, we-got-this-girl bonding experience rather than a call for change within the healthcare industry, which is failing women who are going through menopause.
Having gone through premature induced menopause at thirty-seven years old due to hormonal treatments for breast cancer, I’ve been following these conversations closely. I watched as Drew Barrymore had her first perimenopausal hot flash on-air with Jennifer Aniston, and I listened intently to Maria Shriver talk about the correlation between anxiety and menopause. While I appreciate the courage of these women for speaking out about a topic that has long been shrouded in secrecy—their openness and honesty is even more impressive, considering they work in the youth-obsessed entertainment industry—it’s important to note that this natural biological process can also come with significant medical risks.
When a life-saving hormone treatment hurtled me into premature induced menopause, I had no idea what to expect. At the time, I felt grateful to be alive. The consequences of sudden induced medical menopause weren’t my primary concern. Going into menopause sounded like an abstract concept meant for someone else—like trying to understand childbirth before entering labor. I knew I would no longer get my period (excellent!) and probably have a few hot flashes, as my mother did. I remember her driving me to high school in the dead of a Vermont winter with all the windows down while complaining she was overheating. Back then, I laughed at the absurdity of the situation. But now, twenty-five years later, I understand: hot flashes aren’t funny! They wake me up every night, and I feel like I’m cooking from the inside out.
I was woefully ill-prepared for the intensity of my symptoms, which include rapid mood swings, brain fog, insomnia, night sweats, and severe vaginal atrophy that wreaked havoc on my sex life. My oncologist, and my primary care doctor, failed to educate me about the significant health risks of entering into early menopause, such as the increased likelihood of osteoporosis, depression, stroke, heart disease, and early dementia, to name a few. I’m not blaming them for my symptoms, only for the lack of education and warning.
Why aren’t doctors and oncologists better preparing us, their patients, for what to expect in menopause? I think telling me to “take an over-the-counter Vitamin D supplement” to treat my fragile bones is inadequate. Why didn’t anyone tell me about my increased risk for early-onset Alzheimer’s or the imminent metabolism meltdown? Menopause wreaked havoc on my physical and mental health, and the worst part was how unprepared I was for it. Each new symptom brought on many other health concerns and treating them became my full-time job. I couldn’t turn to my mother for answers because she had passed away from cancer five years before my diagnosis. I became confused, embarrassed, and ashamed about what was happening to my body and felt very alone.
Want more health and science stories in your inbox? Subscribe to Salon’s weekly newsletter The Vulgar Scientist.
Eventually, I took matters into my own hands. I sought information online and I found a supportive community of post-menopausal women who recommended different solutions for my ailments. Before I found these women, I spent hours lurking around random Facebook groups and Reddit threads, searching for advice from strangers. One woman from Ontario even mailed me her homemade lube recipe. It arrived wrapped in pink bubble wrap, inside a discreet package, with no return address. I tried it. (To paraphrase Michelle Obama, “There’s no shame in my menopause game!”) Over the years, I’ve found therapeutics and products that work for me—but none are doctor prescribed or covered by insurance.
We need affordable, effective, and widely available therapies and educational resources for everyone going through menopause. We do not need more menopausal capitalism.
The question remains: Why was I forced to become an internet menopause sleuth? In part because the medical community — oncologists, general practitioners, gynecologists, nurse practitioners, and nurses — are failing to address menopausal symptoms adequately with their patients. Why don’t professionals ask perimenopausal and postmenopausal persons about their vaginal symptoms the minute they enter the examination room? As many as 90% of postmenopausal women experience vaginal dryness, yet no medical practitioner has ever asked me about it. (The fact that Gayle King intoned dry vagina three times during her interview on CBS Mornings is groundbreaking. Seriously.)
Moreover, research shows that medical providers dismiss three out of four women who bring up their symptoms and concerns. While we could all use a little more education on how to be our own health advocates, medical professionals could be doing so much more to normalize these sometimes uncomfortable conversations and end the culture of silent suffering in menopause.
Most of us don’t have the time, money, or resources to research and experiment with various treatments to find the one that works best for them. Some of don’t even have access to decent healthcare. Not to mention the well-documented racial disparity in menopausal health. We need affordable, effective, and widely available therapies and educational resources for everyone going through menopause. We do not need more menopausal capitalism, i.e., celebrities hawking us their products. If anything, we’ve learned from the studies on heart disease, cancer, and exercise science that not enough medical research has gone into unlocking the mysteries of the female body.
Unfortunately, the number of individuals entering menopause at an earlier age keeps increasing. Cancer in young adults is also on the rise. As early detection and treatment continue to improve, more and more people are pushed into chemopause, along with the people who enter early menopause for other reasons. It’s time for more research on managing the symptoms of menopause and open communication about the health risks when estrogen levels radically decline.
Indeed, the public discourse and response around menopause has improved, thanks partly to the outspoken celebrities helping to change the paradigm. But all women, no matter who they are, deserve better and more, both in treatment plans and preventative care (not to mention job security and mental health services). We shouldn’t have to wait for Taylor Swift to enter menopause and write a song about it in order to get everyone’s attention.
I know that when my two young sons become older adults, they will, provided they have health insurance, enter a favorable healthcare world: erectile dysfunction drugs like Viagra are typically covered by insurers, as are vasectomies (which most state Medicaid plans cover). They will also benefit from decades of medical research on the aging male body. But I don’t want my three nieces to go through what I did — the helplessness and isolation of Googling answers about my own body in the dark of night.
I hope that by the time they enter menopause — naturally or medically induced — they’ll have educated themselves about the significant medical risks and symptoms. I want them to live in a world full of medical providers who serve up big helpings of information about their changing female bodies and what to expect once they reach the threshold of menopause. I wish that for them as much as I still wish it for myself and other women going through it.
It goes without saying that I’m grateful to these brave public figures for using their platforms to help change the narrative around menopausal health. But maybe it would also be helpful to create well-written, culturally competent, and widely distributed resources for medical providers along the lines of, “How to Talk to Your Patient Going Through Menopause.” I’m joking — kind of. After all, the conversations which hold the most influence — between doctors and patients — don’t always happen on a stage. Rather, they take place in private examination rooms.
Read more
about menopause

