Mammogram recommendations will save lives, but don’t go far enough
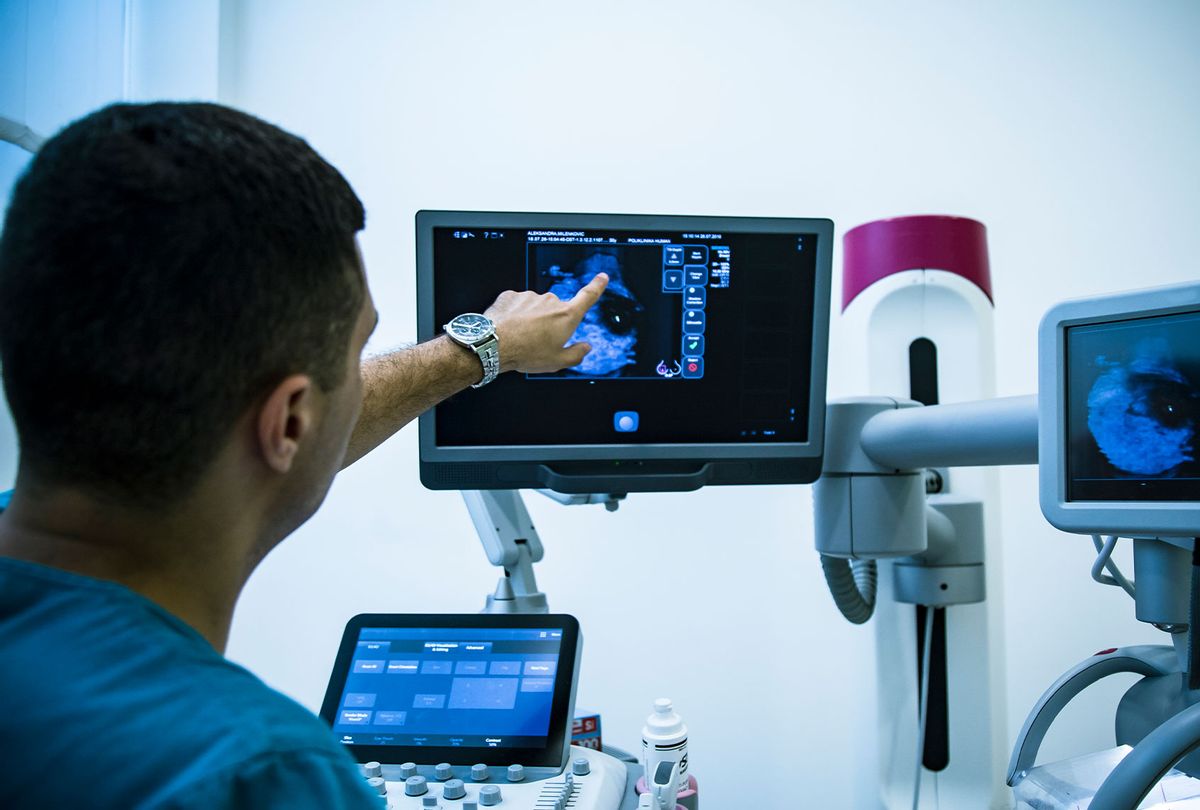
I ignored the mammogram notification that popped up in my health network’s online portal when I turned 40. It was the summer of 2020, and breast cancer seemed like a remote health concern in the context of a pandemic. And I delayed at 41, distracted by work and life — eventually scheduling my first mammogram for late October 2021. The results came back clear, but with a caveat—”the breast tissue is heterogeneously dense, which could obscure detection of small masses” — and a recommendation: a routine follow-up in one year.
I could have delayed again. National guidance on mammograms for people in their forties is mixed, with little clarity on whether to be screened or how often. The American Cancer Society recommends that women with an average risk for breast cancer “have the option” to be screened at age 40 — and, more forcefully, that women between 45 and 54 “should” have annual mammograms. Starting in 2009, though, the U.S. Preventive Services Task Force recommended that mammograms begin at age 50 for women with average risk, and that screenings should occur every two years.
If I had followed that advice, I wouldn’t have scheduled my second mammogram in November 2022. If I had followed that advice, the “focal asymmetry” that appeared in my right breast on that mammogram would have gone undetected, and I wouldn’t have had a follow-up mammogram, ultrasound and biopsy in quick succession.
If I had followed that advice, I wouldn’t have received my breast cancer diagnosis at age 42, just a little over a month after my second annual mammogram.
With no family history of breast cancer, I fell into the “average risk” category prior to my first mammogram, and subsequent testing revealed I have no known genetic markers for cancer of any kind. I did have an elevated risk factor, though: that “heterogeneously dense” breast tissue that appeared in my mammogram. I’m far from unusual in this. A 2014 study estimates that 43 percent of women ages 40 to 74 have dense breast tissue, and multiple studies show that dense breasts are associated with increased risk of breast cancer. In other words, nearly half of all people assigned female at birth are at an increased risk of breast cancer because of the nature of their breast tissue.
This is an important and well-publicized change to the previous recommendation of age 50, but it does not go far enough.
People who have dense breasts could presumably err on the more cautious side of the recommendations then — or talk to their doctors about being screened even earlier than 40. But it isn’t possible to identify dense breast tissue through self-exams, nor can doctors do so through clinical exams. This leaves anyone with an otherwise average risk for breast cancer in a paradoxical situation: the only way to know if you have dense breast tissue — and if you should more aggressively screen for breast cancer — is by getting your first mammogram at a facility that shares information about breast density. The FDA’s March 2023 updates to mammography regulations now require all facilities to notify patients of their breast density, which will ensure that all people who receive mammograms receive this vital information by the end of 2024.
But the mammograms needed to determine both heightened risk and identify suspicious masses must be more consistently and uniformly recommended for all people assigned female at birth when they reach 40. The U.S. Preventive Services Task Force draft recommendations released for public comment this month are a step in the right direction: they suggest “that all women get screened for breast cancer every other year starting at age 40 to reduce their risk of dying from this disease.” This is an important and well-publicized change to the previous recommendation of age 50, but it does not go far enough.
First, the recommendation of every other year is too conservative, especially for women with dense breasts. Second, this recommendation acknowledges but does little to address health disparities for Black women, who have the highest rate of breast cancer incidence before age 40 and whose breast cancer mortality rate is 40 percent higher than White women.
Want more health and science stories in your inbox? Subscribe to Salon’s weekly newsletter The Vulgar Scientist.
Mammograms alone aren’t enough for people at higher risk. In my case, as a White woman with heterogeneously dense breasts, the initial suspicious area on the mammogram was estimated at 9 millimeters, but an MRI just a month later found the “total extent of suspected disease” was more likely 4.3 centimeters — nearly five times larger. Yet MRIs are not recommended in the new draft guidelines for those with dense breasts. Instead, the task force calls for more research on the efficacy of ultrasounds or MRIs.
Some states have introduced or passed legislation to require insurance coverage for these additional screenings, which can be tracked on the American College of Radiology’s Policy Map. In Pennsylvania, where I live, Senate Bill 8 was approved by the governor on May 1, 2023. It requires insurers to cover “all costs associated with one supplemental breast screening every year” for women with increased risk of breast cancer, including heterogeneously dense breast tissue with one other risk category and extremely dense breast tissue with no additional risk categories. While I wouldn’t qualify for additional screening under this new law, it offers an important model for developing a more complete diagnostic picture for people at high risk of breast cancer.
But you shouldn’t have to live in a particular state — or have access to a health network that initiates mammogram reminders at 40 — to receive full health screenings or care. No diagnostic tool is perfect, but annual mammograms are a low-risk assessment mechanism for all people assigned female at birth. For those with elevated risk factors, including both tissue density and race, additional screening via MRIs could catch cancer growth early and lead to improved outcomes for treatment and mortality.
You shouldn’t have to live in a particular state — or have access to a health network that initiates mammogram reminders at 40 — to receive full health screenings or care.
The tumor my surgical team eventually removed was 5.2 centimeters — far larger than that initial area of concern on the mammogram, and large enough to make me wonder what my first mammogram might have missed. I’m more haunted, though, by what my cancer diagnosis would have looked like if I had not started getting mammograms in my early 40s, and if I had not done so annually. Early detection meant that I was able to get a life-saving double mastectomy just a month after diagnosis, that cancer had not yet spread to my lymph nodes and that I am now able to start the hormone therapy that will, my doctors hope, prevent recurrence elsewhere in my body.
Today, I have — in the words of my fantastic surgical oncologist — “no more mamms to gram.” But my peers do, and it is imperative that they receive consistent guidance regarding the benefits of annual mammograms starting at 40, as well as access to the additional screenings necessary to address elevated risk factors.
Read more
about cancer and women’s health

